Nutrition’s Power to Transform Lives – by Reishma Edward 
In March 2023 I embarked on a life-changing sabbatical - a journey filled with compassion, cultural immersion, and invaluable lessons. My destination was Senegal, West Africa, where I had the privilege of volunteering for eight weeks as a dietitian with Mercy Ships.
Mercy Ships deploys hospital ships to low-income countries in sub-Saharan Africa. The humanitarian charity’s mission is to transform the lives of people living with poverty, disfigurement, and disability. Their floating hospitals are a lifeline to communities with limited access to healthcare.
A Glimpse of Senegal
Before my journey, Senegal was a place on the map but my knowledge was limited. Located in West Africa, Senegal's capital is Dakar; home to 17 million people with 38% living on less than 2 dollars a day. Senegal's history of French colonisation and its 1960’s struggle for independence have shaped its unique culture. Wolof, not French, is the predominant spoken language.
After an exhaustive 40-hour journey, I touched down in Dakar where the Global Mercy was docked for 10-months of field service. Jet-lagged but exhilarated, I was greeted warmly by the nutrition team and fellow Kiwis in the international crew. My cabin on deck 5 was spacious and comfortable, shared with a delightful lady from The Netherlands. Three delicious meals a day kept us nourished, and a ship shop and café catered to those seeking additional treats.
Meaningful Work
I worked from Monday to Friday, alongside a dietitian from Australia and two national translators. Our responsibilities included in- and out-patient care, pre- and post-operative assessments and food service. My primary role in pre-operative and post-operative care allowed me to forge meaningful relationships with patients, guiding them through their surgical journeys with crucial nutritional support.
After-hours I enjoyed opportunities to recharge and explore the vibrant Senegalese culture – though being in a Muslim-majority country, I had to adapt my clothing choices accordingly.
Pre-Operative Care
Pre-operatively, we evaluated patients of all ages’ nutritional readiness for surgery, establishing weight goals and timeframes for the malnourished, ensuring they were fit for the transformative procedures ahead.
Our nutritional supplement of choice was Mana, a 500-calorie ready-to-use blend comprising peanut paste, milk, and essential vitamins and minerals - which we often whipped into peanut butter smoothies that were enjoyed by both adults and children.
Patient Journeys
Our patients often travelled long distances to the ship, with some crossing borders from neighbouring The Gambia. Most of them stayed at the Mercy Ships hostel, the HOPE Centre, until they reached their target weight. They often left other children and family members behind, and some were the main income earners. As such, they felt a strong urgency to attain their target weights, receive their surgery, and return home as soon as possible. Patients came for weekly nutrition reviews and were provided with both nutritionally balanced meals and oral nutrition supplements as needed. Insufficient weight gains were challenging, and a significant portion of my time was devoted to encouraging, motivating, and reassuring patients that they were still on track to achieve their weight goals.
One of my most heart-warming experiences was visiting the HOPE Centre and spending quality moments with the paediatric patients. Despite my limited knowledge of Wolof, I quickly discovered that a smile and body language transcended words. We played games, sang songs, and shared hearty laughter. Witnessing the joy in those children's smiles, knowing that their lives were on the cusp of transformation, was profoundly rewarding.
What struck me most about Senegal was the sense of community and togetherness that permeated every aspect of life. Families and communities embraced one another with open arms – which provided vital emotional support for our patients at the HOPE Centre.
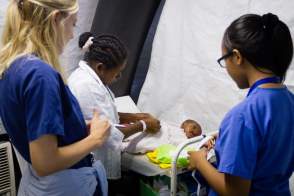
Supporting the Infant Feeding Programme
The Infant Feeding Program provides support to babies born with cleft lip and palate, whose feeding difficulties often lead to malnutrition. We worked closely with mothers, developing feeding plans, offering hands-on guidance, and monitoring progress to prepare infants for surgery while addressing the associated stigma. I worked closely with two translators to assess and educate on various aspects of patients’ feeding practices, including whether they were breast or formula-fed, and what other foods had been introduced. Notably, it was common in West Africa to introduce rice/cereal into milk formula before infants were six months old.
Typically, patients with cleft lip are recommended for surgical intervention when they reach three months and weigh over five kilograms. For those with only a cleft palate, the threshold is one year of age and a weight of over eight kilograms.
After assessing patients, I developed personalised feeding plans, with detailed guidance on hygiene practices, the frequency of feeds, and other essential aspects. Health literacy was often limited, and our sessions needed a practical, hands-on approach. We would demonstrate breast milk expression or formula preparation, closely monitoring the infants' feeding techniques, as well as preparing feeds and assessing the lip-seal and amount of milk consumed. This allowed us to share insights with mums about effective positioning for baby to suckle and reducing risk of chest and ear infections. I also worked with mothers to ensure their own nutritional needs were met. Achieving these goals, and surgical intervention, helped avoid the stigma that mothers and infants often faced in Senegal, where some believed cleft conditions were caused by malevolent spirits.
One stand-out case was a four-month-old baby with both cleft lip and palate, whose mother was unable to breastfeed. The baby was admitted at just 3kgs and it became my mission to help them gain a further 2kgs before surgery. Over weekly nutrition reviews, I forged a meaningful relationship, saw steady gains and developed trust and connection with both mother and baby. Challenges like incorrect formular mixing or feed frequency meant that no weight gain was seen some weeks, and we approached these situations with empathy and care.
While many infants, children and adults successfully reached their goals and underwent surgery, we also encountered heart-breaking situations where surgery had to be declined. These moments were undoubtedly the most emotionally challenging aspects of my role.
Lessons Learned
My volunteer journey with Mercy Ships in Senegal was more than an adventure; it was a transformative experience that left an indelible mark on my life. I learned to embrace diversity, appreciate the resilience of the human spirit, and recognise the pressing need for accessible healthcare in low-income regions. My empathy and compassion deepened, and I witnessed the power of collaboration and teamwork. Most importantly, I gained a profound sense of gratitude for my own privileges and a strong commitment to using them to help others.
Working in this unique healthcare setting was filled with both challenges and triumphs. ‘Navigating the seas’ of pre-operative and post-operative care, I witnessed the incredible power of nutrition to transform lives. As a dietitian, it was about nourishing the body and the soul, forging connections that transcended language barriers. In the end, the smiles of those children and adults with the promise of a brighter future, made it an experience like no other.

Find out more about volunteer dietitian opportunities with Mercy Ships at
www.mercyships.org.nz/make-your-mark/
ABOUT MERCY SHIPS:
Mercy Ships operates hospital ships that deliver free surgeries and other healthcare services to those with little access to safe medical care. An international faith-based organisation Mercy Ships has focused entirely on partnering with African nations for the past three decades. Working with in-country partners, Mercy Ships also provides training to national healthcare professionals and supports the construction of in-country medical infrastructure to leave a lasting impact.
Each year, more than 3,000 volunteer professionals from over 60 countries serve on board the world’s two largest non-governmental hospital ships, Africa Mercy® and Global Mercy™. Professionals such as surgeons, IT professionals, nurses, health trainers, cooks and engineers dedicate their time and skills to accelerate access to safe surgical, obstetric and anaesthesia care.
Mercy Ships was founded in 1978 and has offices in 16 countries including New Zealand, and an Africa Service Centre in Dakar, Senegal.
For more information contact:
Communications Manager
Mercy Ships New Zealand
+64 9 950 4303 (Office)
[email protected]